
Elizabeth Glowacki
PhD
Associate Teaching Professor; Associate Chair for Faculty Governance Public Health and Health Sciences
simulation center
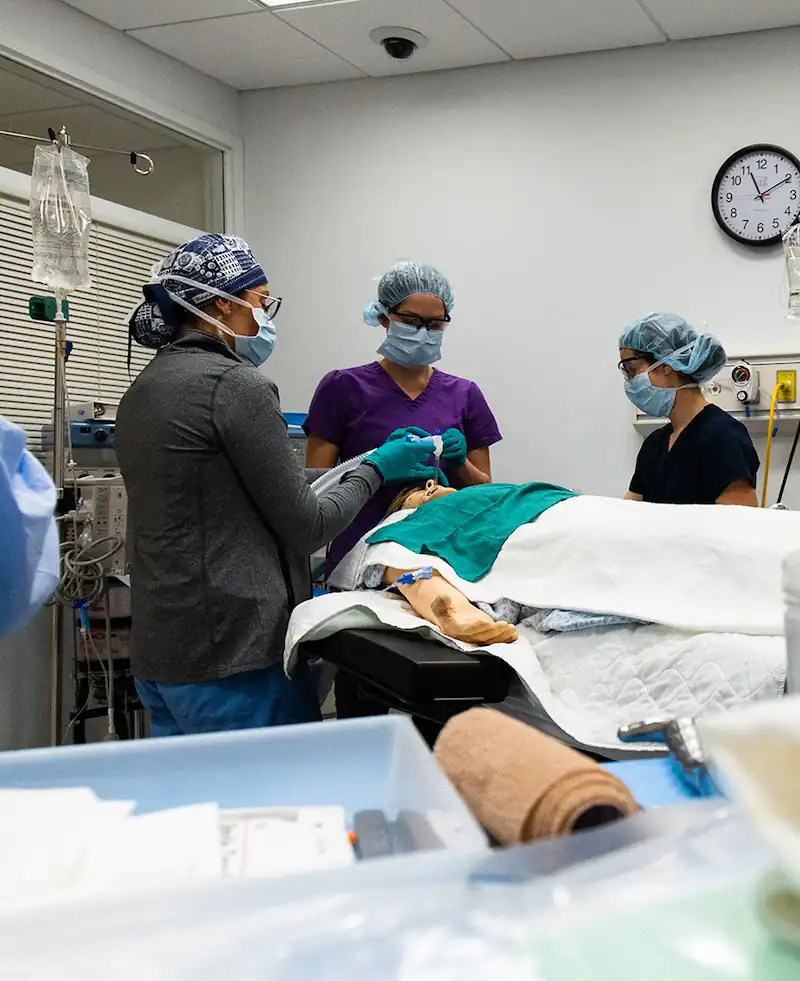
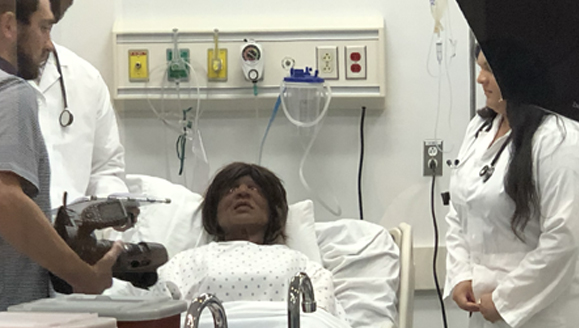

Simulation in health professions education is used to create realistic representation of situations and processes in a wide range of healthcare practice environments, using a variety of activities and technology, ranging from low-technology role-playing to high-fidelity human patient simulators. Through simulation scenarios, real-life clinical situations can be replicated, affording students a heightened and safe learning environment without placing actual patients or the students at risk.
The center is also used for:
If you would like more information, please reach out to Jamie Musler.


The Goldstein Laboratory Suite houses transformable state-of-the-art labs and debriefing rooms. Each lab can be set up as a variety of practice environments including, hospital rooms, operating rooms, exam rooms, office spaces, conference rooms, home care settings or even a dorm room.
Each lab contains video and audio capture technology used to record student experiences as they interact with the latest high-fidelity human patient simulators, patient actors, faculty and other students. Students’ recorded simulation experiences are played back and analyzed during structured debriefing sessions.
Debriefing is a vital component of simulation and a critical piece that drives heightened student learning. It allows for reflection and exploration of the thoughts and emotions behind a learner’s actions. We strive to help all Bouvé students develop the knowledge, skills, attitudes and values that promote patient safety, impact the quality of healthcare, and improve communication for the next generation of health leaders.
Learn about our lab space, the kinds of patient simulators we have, the individuals (standardized patients and actors) who bring life to our learner experiences, and give are patient simulators their voice and personalities.
The Goldstein Simulation Suite is comprises four simulation labs, a control room, a viewing area, and debriefing rooms.

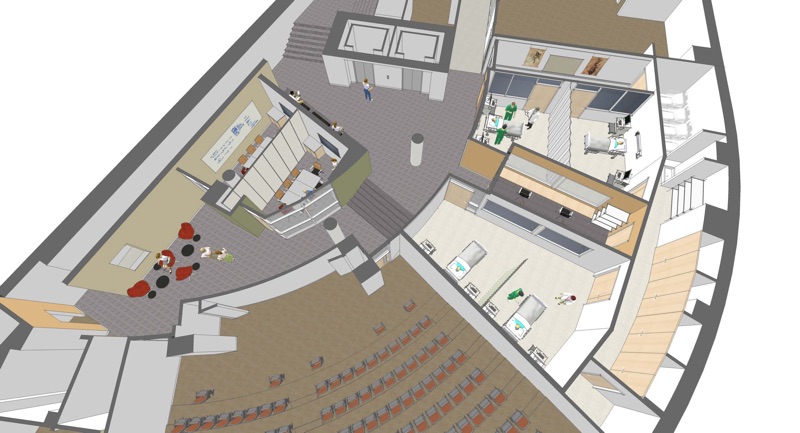
Our labs are designed to be transformed into almost any environment that a scenario calls for.
These are just a few examples of the forms our labs routinely take.
Wired for high resolution video and audio recording, our A/V system allows us to capture a simulation as it happens. The video is then to use during the debriefing session as an element of reflective learning.
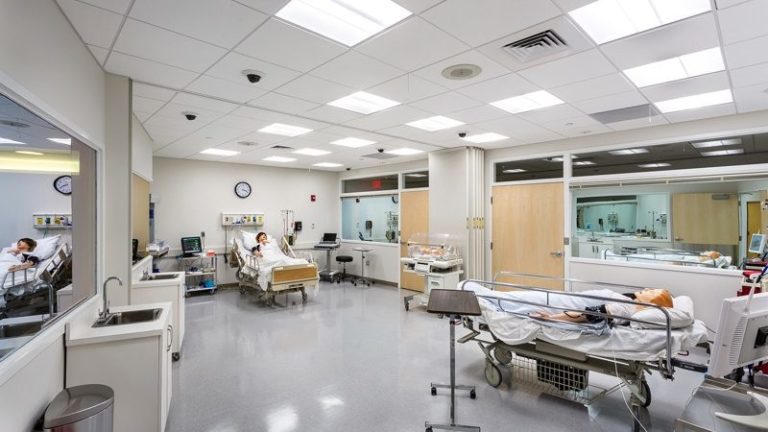
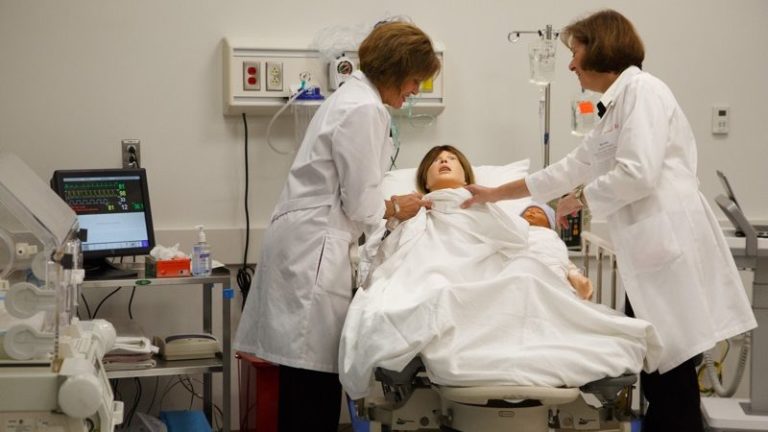
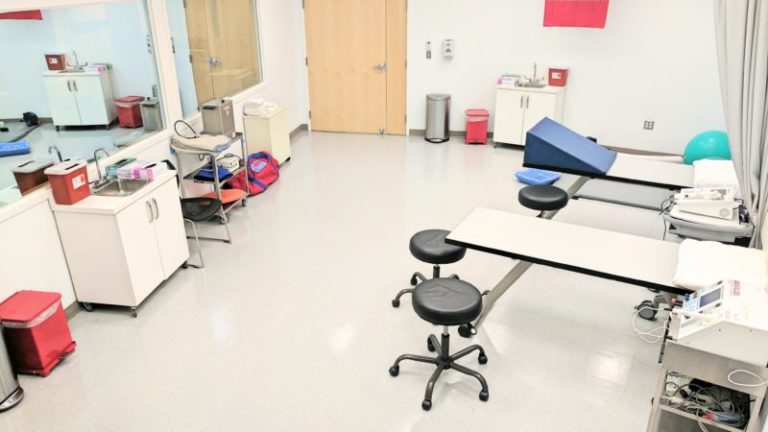
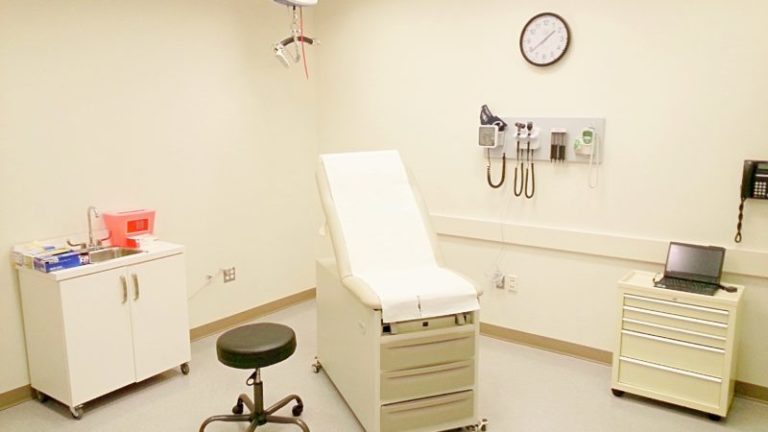

Simulation Center staff and faculty can direct and observe simulations in any of our four labs. Control computers allow for the manipulation of the patient simulators. Faculty can interact with their students as a patient by speaking through the mannequin or employ standardized patients to interact with their students in a given scenario.

Individual or groups of students can view a simulation as it happens. Simulations can be live streamed in one of our debriefing rooms or students can watch and listen from the viewing area. The one-way glass and overhead speakers allow observers to watch without disturbing the students in the learning environment.
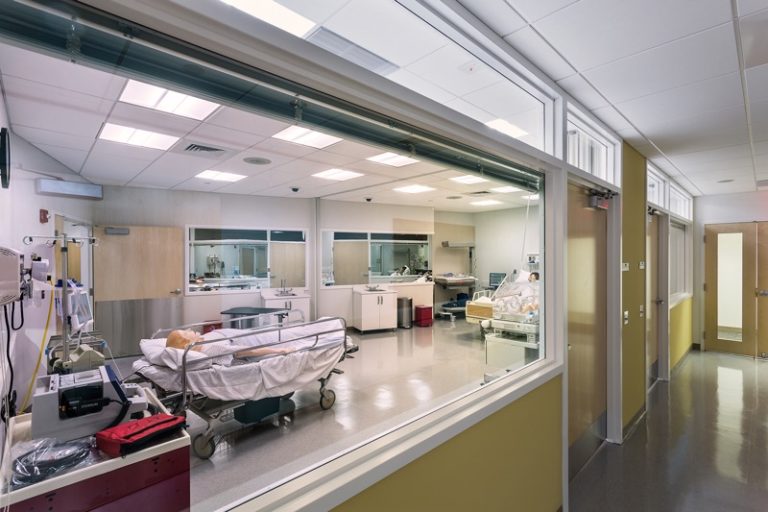
Debriefing is where the learning occurs and is as important as the simulation itself. In the debriefing rooms students reflect on and process their experience in the simulation with guidance from trained debriefers.

At the Goldstein Labs, we use an array of high fidelity human patient simulators to create an environment for our students that is as realistic as possible. Each patient simulator has a wide range of abilities, including light-sensitive eyes that blink, palpable pulses, seizures and more.
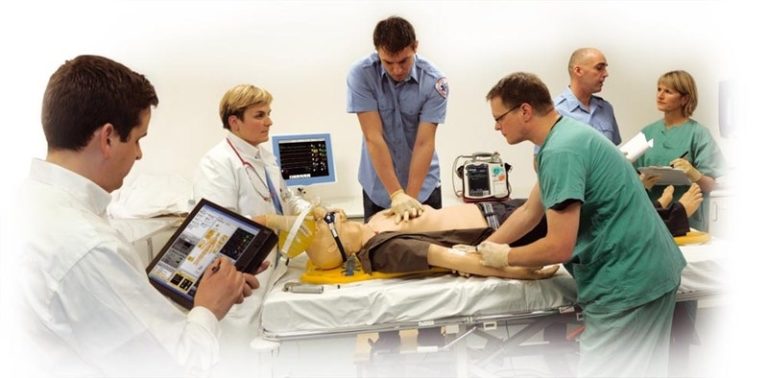
Perhaps our most versatile simulator, SimMan 3G is a fully wireless, multidisciplinary adult patient simulator. SimMan’s wireless features and onboard power supply allow for use in a variety of settings beyond a healthcare environment. At the Goldstein labs we have used these features to simulate the entire chain of care, with first responders treating a patient in a home or office, then transporting the patient to a simulated Emergency Room where the patient is then transferred to a hospital care team.
Sim Man’s technology allows us to replicate almost any sign and symptom to create a highly realistic patient presentation. From the control room, faculty utilize a specialized software interface that allows the simulator to talk, cry, sweat, bleed, convulse, breathe, go into cardiac arrest, have asthma as well as just about any other sign and symptom.

Our obstetric simulator can be used to create patient care experiences in prenatal care, postnatal care, and everything in between
From a routine birth, to a delivery mired by complications, hemorrhage, preeclamptic and eclamptic seizures, caesarian sections, breach delivery, and prolapsed uterus are only a few examples of the challenges that the SimMom can present to the care team.

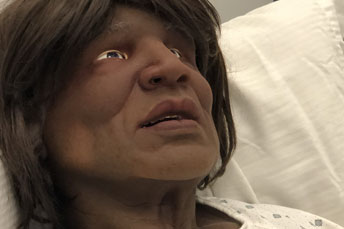
Our range of pediatric simulators allows us to simulate health care crises for a newborn (SimNewB), a 10 month old (SimBaby), and a 6-12 year old child (SimJunior). Our family of pediatric simulators allow us to present students with a wide variety of patient situations including a healthy talking child to an unresponsive critical patient with no vital signs.
Students can gain exposure and clinical experience in a wide variety of pediatric conditions. Students can practice everything from a routine interview and exam, to an urgent care visit, to emergencies such as cardiac arrest, anaphylactic shock, and various forms of trauma. The versatility of these simulators allow us to put our students in scenarios that are as close to reality as possible, leaving them better prepared for actual clinical practice.
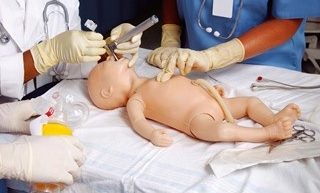

Standardized Patients (SPs) are individuals who are trained to portray a variety of scenarios critical to the development of our students.
Standardized Patients (SPs) were first used in medical education in 1964 by Howard S. Barrows MD. Dr. Barrows was a neurologist at the University of Southern California who introduced the concept of a person trained to portray a patient with specific sign and symptoms for the purposes of educating physicians. The standardized patient training was extremely detailed including the traditional history of a patient as well as the finer details of body language, emotions, personality, and physical findings. These trained patients, became known as standardized patients. Dr. Barrows coached individuals to simulate an actual patient so accurately that the standardized patients could not be detected by experienced clinicians.
Our SP program began in 2013 and currently includes traditional Standardized Patient as well as patient actors. SPs are trained to portray a patient, in a highly consistent and standardized manner assuring each student experiences the same patient interaction. Patient Actors have a similar role portraying patients when there is less of a need for standardization. Patient Actors are also used to portray other critical roles in our simulations including family members, other health care providers, bystanders and other people a healthcare provider may encounter. SPs and patient actors are important components of scenarios that develop critical thinking, professional behaviors, crisis resource management, and communication skills.
Do you need experience to become a SP?
Our SPs are from all walks of life and have a variety of work and personal experiences . SPs typically have excellent communication skills, can remember detailed patient information, have good recall of things they see and hear, and have an interest in educating. It is also helpful to be flexible and available to work any day of the week.
What responsibilities would I have as a SP?
As an SP you will be required to read and memorize case information. You will be expected to be on time and prepared for all assigned scenarios. In some cases, you may be asked to dress and look a certain way to portray the patient or character accurately. You may also be asked to provide feedback and/or asses learner performance. We expect that you will be reliable, take the program seriously, and maintain confidentiality at all times.
How do I apply to be a SP?
SPs are hired as part time employees of the University and are paid hourly for their work. You will be required to complete a hiring application and provide relevant tax and other information including (W-4, M-4, I-9, & Direct Deposit form). In some cases you may be asked to agree to a CORI check.
For more information about becoming a Standardized Patient, please contact:
Dr. Jamie Musler
Director
Arnold S. Goldstein Simulation Labs
The Arnold S. Goldstein Simulation Laboratories Suite engages students and faculty in innovative ways to study and practice clinical reasoning skills, interprofessional education, and health system integration to promote the development of fully functioning interdisciplinary healthcare teams. The Simulation Labs enables participants to research contemporary issues that solve the problems of patients and prepare Bouvé graduates to create the healthy communities of the future. We strive to develop the knowledge, skills, attitudes and values that promote patient safety and improve the quality of health care at all levels of professional achievement.
The Arnold S. Goldstein Simulation Laboratories Suite is a premier, experiential learning environment that unifies interprofessional learning and scholarship to enable a continuum of students and health professionals the opportunity to apply and translate knowledge and skills to real world experiences.

PhD
Associate Teaching Professor; Associate Chair for Faculty Governance Public Health and Health Sciences

DPT
Associate Director of Graduate Affairs; Clinical Professor Physical Therapy, Human Movement, and Rehabilitation Sciences

MS, PA-C
Assistant Clinical Professor Medical Sciences

LPD, ATC
Director, Interprofessional Medical Simulation and The Arnold S. Goldstein Simulation Labs

ScD, CCC-SLP
Associate Professor Communication Sciences and Disorders

BS
Simulation Education Technologist

PharmD
Assistant Dean, Office of Experiential Education; Assistant Clinical Professor Pharmacy and Health Systems Sciences